Stephen’s story
As a sporty 26-year-old, Stephen Thompson was shocked to find himself with a diagnosis of Chronic Thromboembolic Pulmonary Hypertension (CTEPH). This is his story of acceptance, surgery, and learning to live with his experiences.
“My partner Beth and I moved to Newcastle from North Yorkshire at the end of 2017 and I started becoming symptomatic shortly afterwards. I had a number of chest infections through the winter and was coughing up blood. I began struggling to run at my usual pace and to keep up with friends while hiking, and I also found going up steps and staircases difficult.
I was very active before becoming symptomatic, and I think that is why I recognised that something was wrong fairly early on; I was sensitive to any change in my physical capabilities. I went trail running, bouldering, and took part in long distance hikes and hill walking. When these activities started becoming more difficult for no apparent reason, alarm bells started to ring.
I knew something wasn’t right and went to my GP surgery multiple times over six months, seeing a lot of different doctors. It was initially thought I was recovering from a particularly bad chest infection and then I was treated for asthma and given inhalers to use. My symptoms persisted and eventually I was sent for a CT scan which showed embolisms in my lungs. I was put on blood thinning medication immediately but after three months I was told that the medication hadn’t resolved the clots. After more detailed investigations I was diagnosed with CTEPH and referred to a specialist centre.
The diagnosis came as a big shock. I had been proactively working to recover from my symptoms for nine months by this point and had never thought my issue would actually be a chronic illness. However, the specialist nurses guided me through what the diagnosis meant and really helped me by planning out a roadmap for my treatment.
Dealing with the emotional impact
Physical exercise is a big coping mechanism for me and has a great impact on my wellbeing. To be so physically limited felt like my body was letting me down and it was very hard to accept at first. I found it difficult to come to terms with my new limitations, which led to me getting very frustrated and upset at times. I also struggled with the fact that this was an invisible disease; there were no outward signs that I was ill and to others I still looked like a fit 26-year-old. People sometimes didn’t understand that there were things I couldn’t do.
With partner Beth Walking in Wales before diagnosis
Running was out of the question and walking up inclines and steps became increasingly difficult. I was still determined to stay as active as possible, but it was difficult to find a level where I could get out and about but not become ill.
I found a lot of solace in nature during this time, aided through my work with Durham Wildlife Trust, and slowing down allowed me to appreciate many areas of the environment that I had overlooked before. I enjoyed birdwatching and botany as well as making visits to smaller and more accessible nature reserves in my local area and across the country.
Undergoing surgery
Although I was fearful, I knew that pulmonary endarterectomy surgery was the best option for me. However, I was worried that the surgery would have negligible benefits as I was told I possibly had a lot of inaccessible disease.
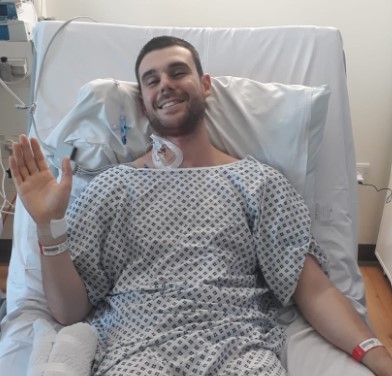
The level of inaccessible disease I was considered to have meant that it was initially decided that I might not be suitable for surgery. When I was told this, it was the most heartbreaking moment of my experience. Thankfully, after further investigations and imagery this decision was reconsidered.
As I waited for a surgery date I experienced doubts and worries. It’s a very scary procedure when you dwell on it, but I just focused on the fact that it was the best treatment for CTEPH. Beth would keep telling me that even if it didn’t cure me entirely it would positively change my condition in some way and that could only be a good thing.
In September 2019 I had my pulmonary endarterectomy surgery at Royal Papworth Hospital which went as smoothly as it possibly could have. After ten days I was allowed to return home to Newcastle.
The road to recovery
Being patient was key in my recovery. I’m thankful to Beth for looking after me through the first few months. I began walking up and down my street for exercise and to build up my strength we would go to a church around the corner which has a convenient flight of seven steps. This was like Everest for me for a while.
About three months after the surgery I started to notice a real improvement in my breathing when walking and going up a flight of stairs. Since then I’ve kept trying longer walks and climbs and have been rewarded as my fitness has recovered and further improved my breathlessness. I can walk by those church steps with a smile now.
I was very lucky to have lots of emotional support through this journey. Beth looked after me and kept my head straight when I became frustrated or depressed with my condition. My family were there for me throughout and everyone at my workplace was also very understanding.
The staff at my specialist centre in Newcastle have all been brilliant and continue to be as I recover from my surgery.
Moving on
These days, I can breathe again! I’m symptomless when exercising; I have no heart palpitations or wheezing, just the feeling of being unfit after nearly two years of limited exercise. I’ve been able to volunteer outdoors and continue with other projects I’ve been working on, with a view to gaining full time employment in the conservation sector. Beth and I have been on a number of hikes in the Cheviot Hills and the Pennines and I’m feeling great. I’m also building back up to a 5km run. It’s amazing how fast my body has recovered from the surgery, and it has also highlighted how severe my symptoms were before.
Through my experience I have fully realised the value of physical health and that you truly don’t know what you’ve got until it’s gone. I’m just lucky enough to have got it back! I also came to terms my own mortality when facing major surgery, and also when the prospect of my surgery was unclear.
With friends in the Lake Disrtict With his brother on the moors
Spending so much time in hospital for investigations, surgery and clinics has given me a massive appreciation for the health service and the level of knowledge and skills required.
I have also learned how to slow down and appreciate the smaller things, whether that might be a study of nature or my relationships with family and friends.
I’m still not back to normal and maybe I never will be really, after going through such a traumatic experience. I take a positive view of this though as I have learned a lot about myself from it.
Although I no longer have PH I’m still not out of the woods with my health in regards to damage to my lungs, clotting and infection risks, so that still plays on my mind. However, I’m taking the best care of myself that I can.”
“You can make the best of a bad situation”
Learning from his own experiences, Stephen has the following advice for anyone newly diagnosed with pulmonary hypertension
Keep as active and healthy as possible. Try and find or adapt hobbies and passions to fit with your limitations.
Be gently persistent with healthcare support for the information you need to understand your condition. Read up on your health condition or procedures yourself. Although scary at first, it will help put your mind at ease in the long run.
Make sure you get the financial support you need! I had to put my misplaced pride to one side in order to get the financial support I was entitled to.
Try to talk to people about your condition. Most people will understand and offer support if they can.
You can make the best of a bad situation. When I was made to switch to desk based work, I was disappointed but it has actually led to me building a whole new set of skills and experiences that I would have missed out on otherwise. I also made use of having more time to pursue other interests such as horticulture, photography, and film.




















